In a groundbreaking clinical trial, a revolutionary tiny wireless chip, when paired with advanced smart glasses, has demonstrably restored partial vision for individuals battling the advanced stages of age-related macular degeneration (AMD). This innovative technology, a culmination of decades of dedicated research and development, has achieved a monumental feat: enabling individuals with otherwise untreatable vision loss to once again perceive shapes and patterns, a level of vision previously considered unattainable by prosthetic devices. The study, a collaborative effort spearheaded by Stanford Medicine and an international consortium of leading medical institutions, has revealed that a remarkable 27 out of 32 participants regained the crucial ability to read within a year of receiving the implant. This significant advancement, detailed in the prestigious New England Journal of Medicine on October 20th, heralds a new era in the quest to restore functional vision and combat the devastating effects of blindness.
The implant, christened PRIMA, represents a paradigm shift in the field of visual prosthetics. Unlike earlier attempts that primarily offered light sensitivity, PRIMA delivers "form vision," allowing patients to distinguish objects and their configurations. Dr. Daniel Palanker, a distinguished professor of ophthalmology at Stanford Medicine and a co-senior author of the study, emphasized the unprecedented nature of this achievement, stating, "All previous attempts to provide vision with prosthetic devices resulted in basically light sensitivity, not really form vision. We are the first to provide form vision." The research was co-led by Dr. José-Alain Sahel, professor of ophthalmology at the University of Pittsburgh School of Medicine, with Dr. Frank Holz of the University of Bonn in Germany serving as the lead author, underscoring the global reach and collaborative spirit behind this breakthrough.
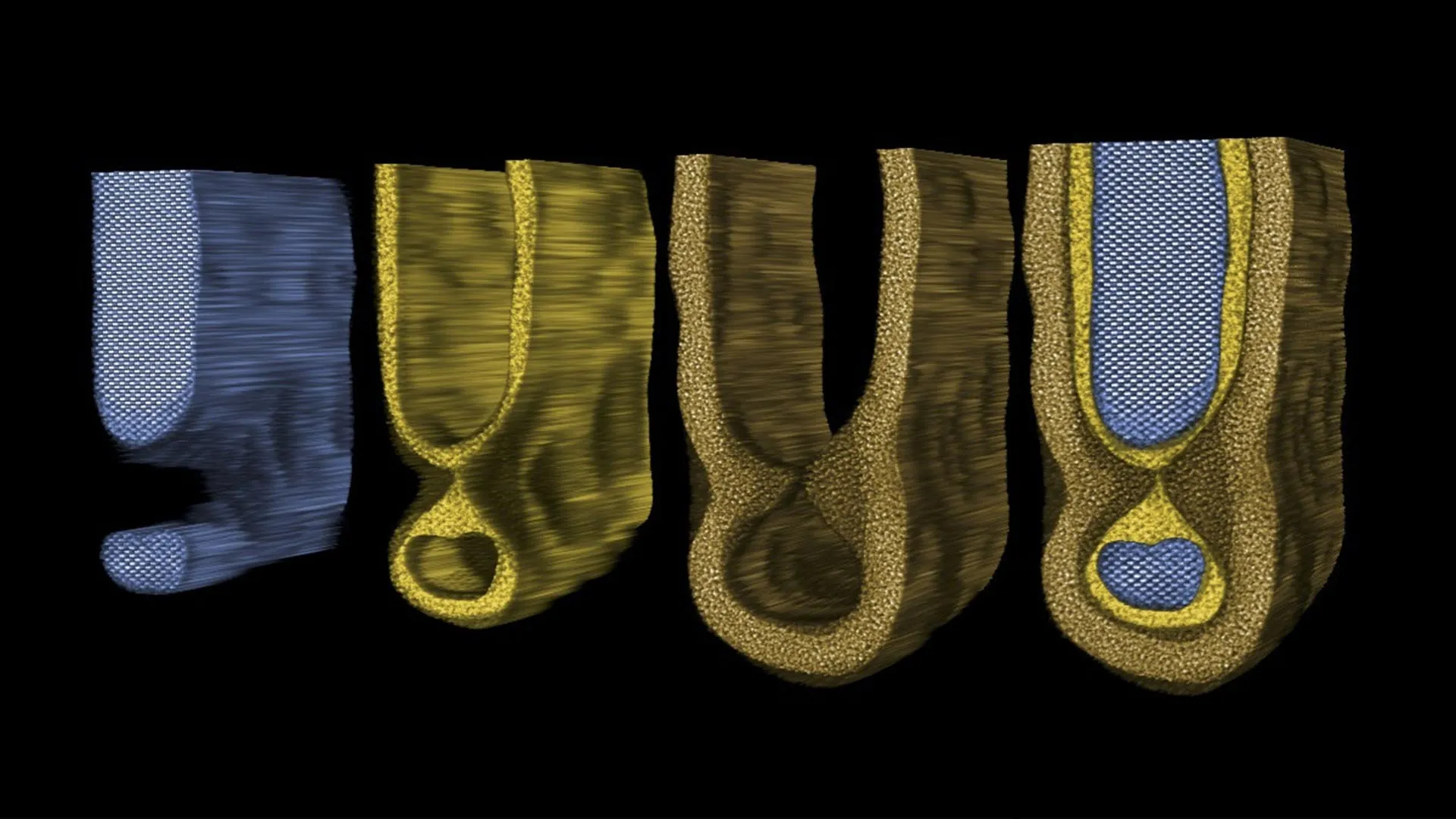
The PRIMA system ingeniously comprises two core components: a miniature camera integrated into a pair of specialized glasses and a wireless chip surgically implanted in the retina. The camera meticulously captures visual information from the environment and transmits it via infrared light to the implanted chip. This sophisticated implant then meticulously converts the infrared signals into electrical impulses, effectively substituting for the damaged photoreceptor cells that are the eye’s natural light detectors. These electrical signals are then relayed to the brain, where they are interpreted as visual input. This elegant design bypasses the compromised photoreceptors, leveraging the remaining intact neural pathways within the retina to convey visual data.
The journey to this remarkable success was a long and arduous one, spanning two decades of relentless scientific inquiry. Dr. Palanker first conceptualized the idea two decades ago while immersed in research involving ophthalmic lasers for treating eye disorders. "I realized we should use the fact that the eye is transparent and deliver information by light," he recalled. This foresight led to the development of numerous prototypes, extensive animal testing, and ultimately, the initial human trials that paved the way for the current groundbreaking study. The realization of this vision, a device first imagined in 2005, has now been remarkably validated in patients.
The clinical trial focused on individuals suffering from the advanced stages of age-related macular degeneration, specifically geographic atrophy. This debilitating condition progressively erodes central vision, impacting over 5 million people worldwide and serving as the primary cause of irreversible blindness in older adults. In AMD, the light-sensitive photoreceptor cells in the central retina deteriorate, leaving individuals with only limited peripheral vision. However, a critical aspect of this disease is that many of the retinal neurons responsible for processing visual information often remain functional. PRIMA ingeniously exploits these surviving neural structures.
The implant itself is remarkably compact, measuring a mere 2 by 2 millimeters. It is precisely positioned in the area of the retina where the photoreceptors have been lost due to the disease. A key distinction of the PRIMA chip is its response to infrared light, emitted by the glasses, rather than visible light that natural photoreceptors detect. Dr. Palanker explained the rationale behind this choice: "The projection is done by infrared because we want to make sure it’s invisible to the remaining photoreceptors outside the implant." This strategic design allows patients to seamlessly integrate their natural peripheral vision with the newly restored prosthetic central vision, significantly enhancing their spatial awareness, orientation, and mobility. "The fact that they see simultaneously prosthetic and peripheral vision is important because they can merge and use vision to its fullest," Palanker noted.
Furthermore, the PRIMA device is photovoltaic, meaning it generates its own electrical current solely from light. This ingenious self-powering mechanism eliminates the need for external power sources or cumbersome cables that would extend outside the eye, a significant advantage over earlier prosthetic eye designs. This wireless, self-contained nature ensures greater patient comfort and safety, allowing for discreet placement beneath the retina.
The recent trial enrolled 38 participants, all over the age of 60, who had been diagnosed with geographic atrophy due to AMD and possessed visual acuity worse than 20/320 in at least one eye. Following the surgical implantation of the chip in one eye, patients commenced using the specialized glasses four to five weeks later. While some individuals could discern patterns immediately, all participants experienced a notable improvement in their visual acuity over several months of dedicated training. "It may take several months of training to reach top performance — which is similar to what cochlear implants require to master prosthetic hearing," Dr. Palanker observed, drawing a parallel to the learning curve associated with other sophisticated sensory prosthetics.
Of the 32 patients who completed the rigorous one-year trial, an impressive 27 achieved the ability to read. Moreover, 26 participants demonstrated clinically meaningful improvement in their visual acuity, defined as the capacity to read at least two additional lines on a standard eye chart. On average, participants experienced an improvement of five lines on the eye chart, with one individual achieving an extraordinary improvement of twelve lines. The practical impact of this restored vision was profound, enabling participants to engage in daily activities such as reading books, deciphering food labels, and navigating public transportation by reading subway signs. The smart glasses offered customizable features, including adjustable contrast, brightness, and magnification up to 12 times, further enhancing their utility. The overwhelming satisfaction with the device was evident, with two-thirds of participants reporting medium to high user satisfaction. While 19 participants experienced transient side effects, including ocular hypertension, peripheral retinal tears, and subretinal hemorrhage, these were generally not life-threatening and resolved within two months.
Looking ahead, the PRIMA device, currently providing black-and-white vision, is on the cusp of further advancements. Dr. Palanker is actively developing software to introduce a full spectrum of grayscale, a crucial step for tasks like face recognition, which he identified as the second most desired capability by patients after reading. The pursuit of higher resolution vision is also a key focus, with ongoing engineering of chips featuring smaller pixels. The current iteration boasts 378 pixels, each 100 microns wide. However, a next-generation chip, already showing promise in animal trials, aims for pixels as small as 20 microns wide, dramatically increasing the pixel count to 10,000 per chip. This enhanced resolution, coupled with electronic zoom, could potentially restore vision close to 20/20. Dr. Palanker is also keen to explore the applicability of the PRIMA device for other forms of blindness caused by photoreceptor loss. The future promises not only improved visual acuity but also sleeker, more aesthetically pleasing glasses to accompany these advanced chips. The collaborative effort behind this remarkable achievement involved a vast network of researchers from institutions including the University of Bonn, Germany; Hôpital Fondation A. de Rothschild, France; Moorfields Eye Hospital and University College London; Ludwigshafen Academic Teaching Hospital; University of Rome Tor Vergata; Medical Center Schleswig-Holstein, University of Lübeck; L’Hôpital Universitaire de la Croix-Rousse and Université Claude Bernard Lyon 1; Azienda Ospedaliera San Giovanni Addolorata; Centre Monticelli Paradis and L’Université d’Aix-Marseille; Intercommunal Hospital of Créteil and Henri Mondor Hospital; Knappschaft Hospital Saar; Nantes University; University Eye Hospital Tübingen; University of Münster Medical Center; Bordeaux University Hospital; Hôpital National des 15-20; Erasmus University Medical Center; University of Ulm; Science Corp.; University of California, San Francisco; University of Washington; University of Pittsburgh School of Medicine; and Sorbonne Université. The study received vital funding from Science Corp., the National Institute for Health and Care Research, Moorfields Eye Hospital National Health Service Foundation Trust, and University College London Institute of Ophthalmology, underscoring the significant investment and commitment required to bring such life-changing technologies to fruition.